Arch. Endocrinol. Metab. 2026;70(special issue 1): e250095
Hypercoagulability in Cushing’s syndrome: past, present, future
DOI: 10.20945/2359-4292-2025-0095
ABSTRACT
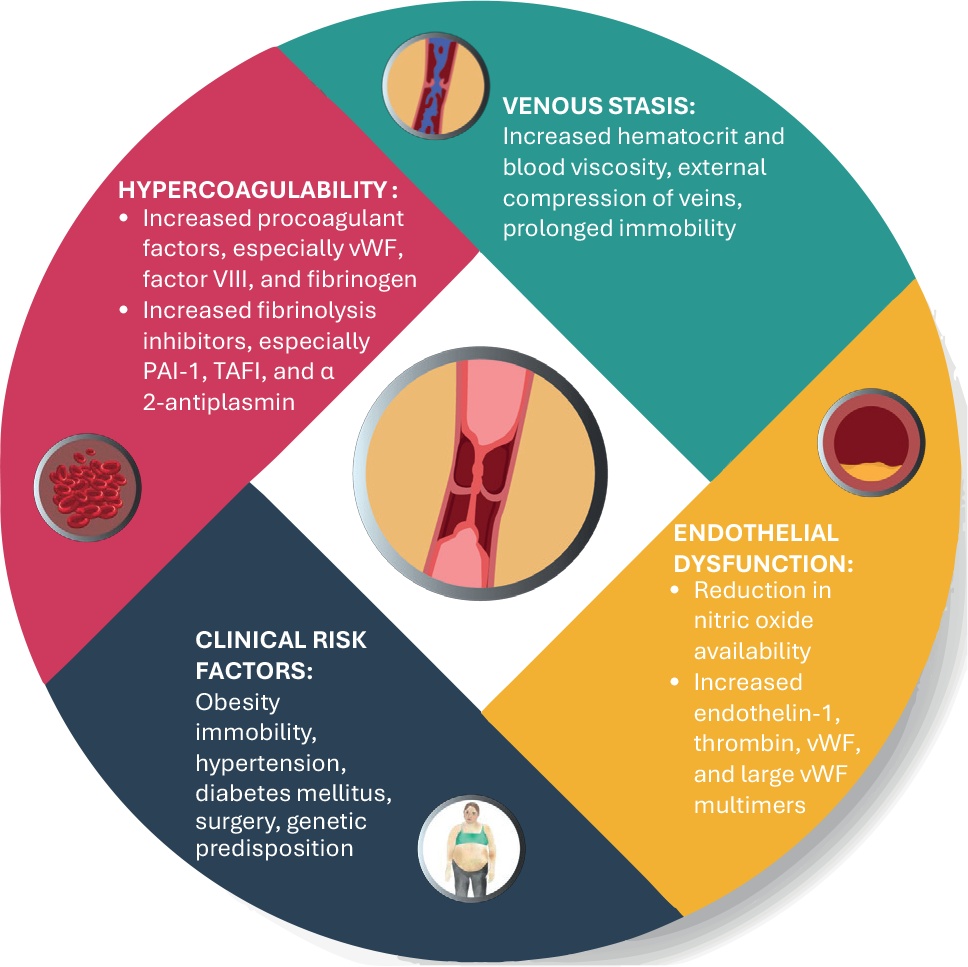
Cushing’s syndrome is a chronic disorder characterized by prolonged glucocorticoid exposure, leading to significant multisystem complications. Multiple epidemiological studies have demonstrated a substantially elevated risk of venous thromboembolism in patients with Cushing’s syndrome, including deep vein thrombosis and pulmonary embolism, particularly during active disease, the perioperative period, but more importantly also after biochemical remission. Hypercortisolism promotes a hypercoagulable state through multiple mechanisms, including persistent endothelial dysfunction, increased procoagulant factors such as von Willebrand factor and factor VIII, impaired fibrinolysis, and venous stasis. Additionally, common comorbidities in Cushing’s syndrome, such as obesity, hypertension, and diabetes, further amplify thrombotic risk. Given these findings, recent consensus recommends thromboprophylaxis for most patients with Cushing’s syndrome, with anticoagulation therapy initiated at diagnosis, continued perioperatively, and extended post-remission when appropriate in patients both after surgery and also in patients on medical therapy. Low molecular weight heparin is the preferred anticoagulant, while direct oral anticoagulants require further investigation in patients with Cushing’s syndrome. Despite these recommendations, clinical practice varies significantly across centers and countries, highlighting the need for standardized thromboprophylaxis protocols. Future research should focus on refining risk stratification models, optimizing prophylaxis duration, and evaluating the long-term thrombotic risk in Cushing’s syndrome remission. Additionally, studies exploring the safety and efficacy of direct oral anticoagulants and personalized medicine approaches through biomarker-driven strategies may further improve patient outcomes. Addressing these gaps will enhance thromboembolism prevention strategies in Cushing’s syndrome and ultimately may reduce morbidity and mortality in this high-risk population.
Keywords: Cushing’s syndrome; Thromboembolism; Thrombophilia